Legionnaires’ disease – causes, route of infection, symptoms and treatment
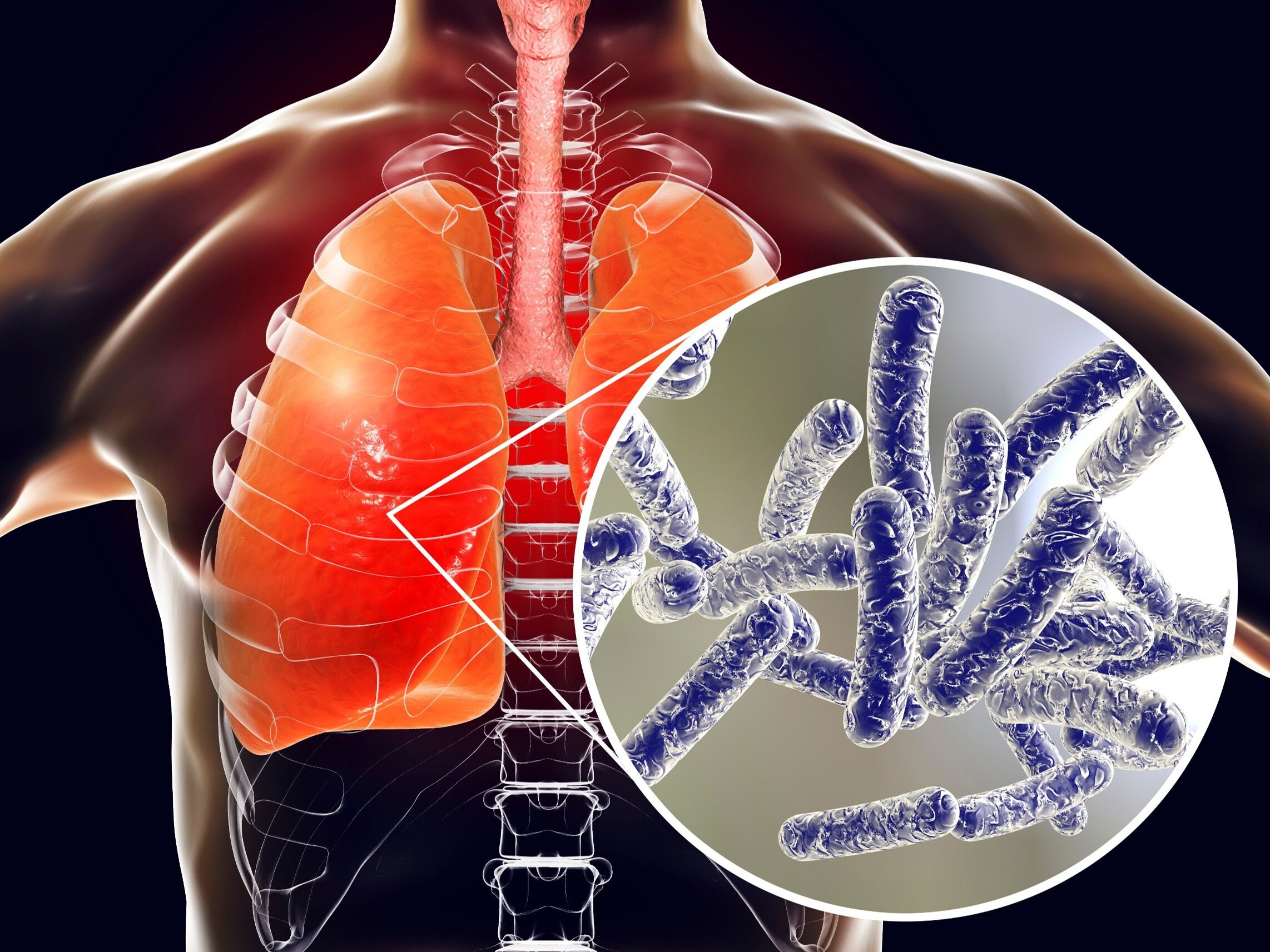
Legionnaires’ disease (legionellosis) can lead to respiratory failure and death. It develops as a result of infection with the Legionella Pneumophila bacterium. The family of gram-negative aerobic bacteria of the genus Legionella includes nearly 50 species of bacteria of various virulence. Legionella Pneumophila is the most dangerous member of this family, causing acute pneumonia. When are we exposed to Legionella Pneumophila infection? We explain.
- Legionnaires’ disease – basic information
- Legionnaires’ disease – how does it get infected?
- Where does Legionella Pneumophila live?
- Where is Legionella Pneumophila infection most common?
- Legionnaires’ disease symptoms
- What increases the risk of legionnaires’ disease?
- Legionnaires’ disease treatment
In 1976, the first mass infection of Legionella Pneumophila occurred during a reunion of World War II veterans of one of the American legions. 186 people fell ill at that time; 34 people died of severe pneumonia. At the time, it was not known what caused the infection. The bacterium detected in the bodies of the patients was named “Legionella” to commemorate the first victims of the infection.
Although nearly 50 years have passed since the first group infection, Legionella Pneumophila is still becoming the cause of serious respiratory infections. Today, however, it is known what is the source of infection and how it occurs. Legionnaires’ disease is the most severe form of infection. The mild form of Legionnaires’ disease – Pontiac fever – is not life-threatening. Pontiac fever causes mild flu-like symptoms. With Pontiac fever, the symptoms go away on their own.
It is worth learning more about Legionnaires’ disease and other infections that are caused by Legionella bacteria, because the disease can occur, among others, in while staying at the hotel.
Legionnaires’ disease – basic information
Legionella Pneumophila is the most common Legionella bacteria. We are exposed to this microorganism both in the natural environment and in public facilities, e.g. in hospitals and accommodation facilities.
In the natural environment, Gram-negative Legionella are found in most freshwater, such as rivers, lakes and hot springs, as well as in the soil. Legionella bacteria live in water with a temperature of 20-55 degrees Celsius. In water whose temperature is lower than 20 degrees or higher than 55 degrees, bacteria are present, but they do not multiply. In water with a temperature of 70 degrees, legionella bacteria die.
Due to the wide temperature range tolerated by Gram-negative aerobic bacilli, the risk of infection increases. Bacteria can start to multiply, e.g. when heating cold water with e.g. electric and gas boilers.
Legionnaires’ disease – how does it get infected?
The infection with the Legionella Pneumophila bacterium occurs through droplets – the bacteria enter the human body when inhaling water aerosol. Gastrointestinal infection is rare. Infection is also possible through open wounds, e.g. during surgical procedures.
Importantly, the reservoir of Legionella Pneumophila bacteria are not humans and animals. Legionnaires’ disease and other diseases caused by gram-negative aerobic bacilli are not transmissible from person to person.
Where does Legionella Pneumophila live?
Optimal conditions for the existence of Gram-negative aerobic Legionella bacteria are provided by, among others:
-
cooling towers,
-
swimming pools,
-
fountains,
-
water curtains,
-
jacuzzi,
-
SPA,
-
water filters.
Legionella Pneumophila bacteria can also live in air humidification systems, e.g. home humidifiers and nebulizers, air conditioning systems and water installations – due to the wide range of tolerated temperatures, they can be found in hot water and cold tap water installations. It happens that microorganisms causing Legionnaires’ disease are detected in thermal springs, as well as in compost and fertilizer mixtures.
The most common sources of infection are neglected water systems and improperly cleaned air humidification and air conditioning systems. Infections are favored by unstable operation of utility water heating systems, as well as insufficient water circulation, e.g. in installations used seasonally.
Where is Legionella Pneumophila infection most common?
In most cases, Legionnaires’ disease affects people who use e.g. from recreational facilities, sports clubs, hotels and other accommodation facilities. Infection occurs less frequently in hospitals and through contact with medical equipment, in restaurants and when using natural water reservoirs.
Potential threats are all improperly serviced water, air-conditioning and ventilation systems. We are exposed to infection not only in public spaces or when traveling around the world, but also in our own home and car. All devices and installations containing water should be systematically cleaned and properly serviced. It happened that the source of serious infection were, for example, home air humidifiers, which we willingly use during the heating season.
Group infections of Legionnaires’ disease are most often associated with staying in hotels, campsites, campsites, cruise ships and recreational facilities. The growth of Legionella Pneumophila bacteria is favored by the seasonal use of old water systems. What is important – Legionella Pneumophila bacteria prefer an environment rich in nutrients – they are more common, e.g. in pipes with mineral deposits.
As already mentioned, infection occurs by droplet infection. We can become infected when we inhale water aerosol while taking a shower or breathe air that contains droplets of contaminated water.
Legionnaires’ disease symptoms
Legionnaires’ disease leads to severe pneumonia. It usually takes 2-10 days from infection to the first symptoms of the disease.
The first symptoms of the disease are high fever, chills, headaches and general malaise. The typical course of Legionnaires’ disease is also associated with respiratory symptoms, including:
-
dry cough,
-
pain in the chest,
-
breathing disorders.
In the course of the disease, there are also other symptoms of pneumonia, neurological symptoms, which include impaired consciousness, as well as digestive system symptoms, such as abdominal pain and vomiting.
The pulmonary form of Legionnaires’ disease can be fatal. A person with Legionnaires’ disease pneumonia requires hospitalization. According to the WHO, 20,000-100,000 people die each year due to Legionella Pneumophila infection. Still, a serious problem is the rapid diagnosis of the disease. It is estimated that 15-20% of cases of Legionnella infection result in death due to respiratory failure.
In extreme cases, in addition to pneumonia, there may also be symptoms of infection of other organs – extrapulmonary Legionnaires’ disease can lead to disseminated coagulation syndrome or sepsis.
Pontiac fever has a milder course. In this case, symptoms appear about 24-48 hours after infection. The symptoms of Pontiac fever are typical flu-like symptoms, which include:
-
high fever,
- headache,
- muscle and joint pain,
-
feeling broken
-
chills.
Gastrointestinal symptoms are less common with Pontiac fever. The symptoms subside spontaneously within a few days.
What increases the risk of legionnaires’ disease?
Factors that increase the risk of developing and severe disease have been identified – bacteria from the Legionella family differ in terms of virulence, but the proper functioning of the immune system has a significant impact on the course of infection.
Risk factors include:
-
age – the elderly are particularly at risk of infection,
- respiratory diseases, e.g. lung diseases related to smoking,
-
congenital and acquired immunodeficiency,
-
kidney disease,
-
alcohol abuse,
-
diabetes.
Legionnaires’ disease treatment
Infections caused by Legionella Pneumophila and other Legionella bacteria are treated with antibiotics. Important! All cases of illness caused by Legionella bacteria are subject to mandatory notification.
Sources:
https://epibaza.pzh.gov.pl/story/legioneloza.
https://legionella.pl/choroba-legionistow/.
https://www.gov.pl/web/gis/legioneloza-choroba-legionistow.
Zdzisław Dziubek, Infectious and parasitic diseases, Wydawnictwo Lekarskie PZWL, Warsaw, 2012.
Virella G., Microbiology and infectious diseases, Wydawnictwo Medyczne Urban & Partner, Wrocław, 2020.






